Chia Seeds for Liver Health: What the Research Really Says About Fatty Liver
Chia Seeds for Liver Health: What the Research Actually Says About MASLD & Fatty Liver.
Nutrition & Liver Health — Evidence-Based Guide — Updated 2026.
Liver Health / MASLD
A genuine deep-dive into the science, the limitations, the case studies, and the one thing most chia seed articles refuse to tell you.
By Nutrition Research Team—10 min read • 2,100 words—Medically reviewed 2025
Medical Disclaimer: This article is for informational purposes only. It does not constitute medical advice. If you have been diagnosed with MASLD, metabolic-associated steatohepatitis (MASH), or any liver condition, please work with a qualified hepatologist or registered dietitian before making dietary changes.
My aunt was diagnosed with MASLD in late 2022. Her doctor handed her a one-page printout and said, “Lose weight, reduce sugar, exercise more.” She went home, opened Google, and found seventeen articles telling her to eat chia seeds. Not one of them told her why. Not one of them cited a single study. I wrote this for her — and for everyone else who deserves an honest answer.
What You Will Find Here
- What is MASLD, and Why Does Diet Matter So Much?
- What Chia Seeds Actually Contain
- The Science: What Studies Actually Show
- Three Key Mechanisms That Benefit the Liver
- The Honest Limitations Nobody Talks About
- How to Use Chia Seeds for Liver Support
- Three Real-World Case Outcomes
- Chia vs Other Liver-Supportive Foods
- Frequently Asked Questions
- Final Verdict
38%of global adults are estimated to have some degree of hepatic steatosis
10gof fibre in just 28g of chia seeds (one serving)
2023Year NAFLD was officially renamed MASLD by major hepatology societies
What Is MASLD and Why Does Diet Matter So Much?
MASLD stands for Metabolically Associated Steatotic Liver Disease. If you knew it as NAFLD — Non-Alcoholic Fatty Liver Disease — the name changed in 2023 when the American Association for the Study of Liver Diseases and the European Association for the Study of the Liver agreed the old name was both stigmatising and imprecise. The new name tells you something crucial: this is fundamentally a metabolic condition, not just a liver condition.

Fat accumulates in liver cells when the body’s ability to process glucose and lipids breaks down. Insulin resistance is the engine driving most cases. The liver, trying to do too many jobs at once, ends up storing fat it cannot burn fast enough. Over time, that fat causes inflammation. Inflammation leads to fibrosis. Fibrosis, unchecked, becomes cirrhosis. The progression is slow, often silent, and largely reversible in early stages with the right interventions.
Here is what most people miss entirely. Diet does not just reduce the calories loading the liver. It changes the microbial environment in the gut, which talks directly to the liver via the portal vein. It modulates inflammatory pathways. It shifts insulin sensitivity at the cellular level. That is why certain foods show up repeatedly in liver health research — not because they are magic, but because they influence multiple mechanisms simultaneously.
Real Experience
My aunt’s hepatologist told her the most evidence-backed intervention for early MASLD is a 7 to 10 percent reduction in body weight. But he also said this: “The foods you choose matter beyond the calories. They change how your gut communicates with your liver.” That single sentence made everything click. Chia seeds started making sense to her once she understood gut-liver communication.
What Chia Seeds Actually Contain
Before diving into liver-specific research, you need to understand why chia seeds are even in the conversation. The nutritional profile is genuinely unusual for a single food.

Nutritional Profile — Per 28g Serving (approx. 2 tablespoons)
Dietary Fibre (total)10g
36% of the daily recommended intake — both soluble and insoluble types present
ALA Omega-3 Fatty Acids5.1g
Highest plant-based omega-3 source by weight, though conversion to EPA/DHA is limited
Protein4.7g
Complete amino acid profile — rare for a plant food
Polyphenols (chlorogenic acid, caffeic acid)Significant
Antioxidant capacity measured as high in ORAC testing
Magnesium 95 mg (23% DV)
Magnesium deficiency is common in MASLD patients — this matters
Three components stand out for liver health specifically: the soluble fibre fraction, the omega-3 fatty acids, and the polyphenol content. Each acts on different aspects of the MASLD pathology. That multi-mechanism action is what makes chia seeds more interesting than a simple “high-fibre food.”
The Science: What Studies Actually Show

Let me be direct about something. Chia seed research is promising, but the evidence base is not as strong as wellness content online suggests. Most studies are animal models, small human trials, or observational data. That does not make them worthless. It means we should calibrate our expectations correctly.
The Most Relevant Human Evidence
A 2021 randomised controlled trial published in the journal Nutrients examined chia seed supplementation in patients with type 2 diabetes and metabolic syndrome — two conditions that overlap heavily with MASLD. Over 12 weeks, the intervention group consuming 25 grams of chia seeds daily showed significant reductions in triglycerides (average reduction of 22 percent), fasting blood glucose, and waist circumference compared to the control group. Triglyceride reduction matters enormously for fatty liver because hepatic triglyceride accumulation is a primary driver of steatosis.
A 2022 study in Frontiers in Nutrition specifically examined the effect of dietary fibre patterns on liver fat using MRI imaging. While not chia-specific, it demonstrated that soluble fibre intake above 8 grams per day was associated with meaningful reductions in liver fat percentage over six months. One standard serving of chia seeds gets you 10 grams alone.
Key Study Finding
A 2020 animal study published in Food and Chemical Toxicology fed chia seed-supplemented diets to mice with induced hepatic steatosis. After eight weeks, the supplemented group showed reduced hepatic lipid accumulation, lower oxidative stress markers (specifically MDA levels), and upregulated expression of genes involved in fatty acid oxidation. Notably, liver histology showed less inflammatory cell infiltration in the chia group. Animal data do not translate directly to humans, but these mechanisms are biologically plausible in the human liver context.
Three Key Mechanisms That Benefit the Liver
Mechanism One: Soluble Fibre and Gut-Liver Communication
The soluble fibre in chia seeds — primarily mucilage, which is what creates that distinctive gel when chia is soaked in water — ferments in the large intestine to produce short-chain fatty acids (SCFAs). The most studied of these is butyrate. SCFAs travel directly to the liver via the portal vein and have been shown to reduce hepatic inflammation, improve insulin sensitivity in hepatocytes (liver cells), and modulate the lipogenesis pathway that drives fat accumulation in the liver.
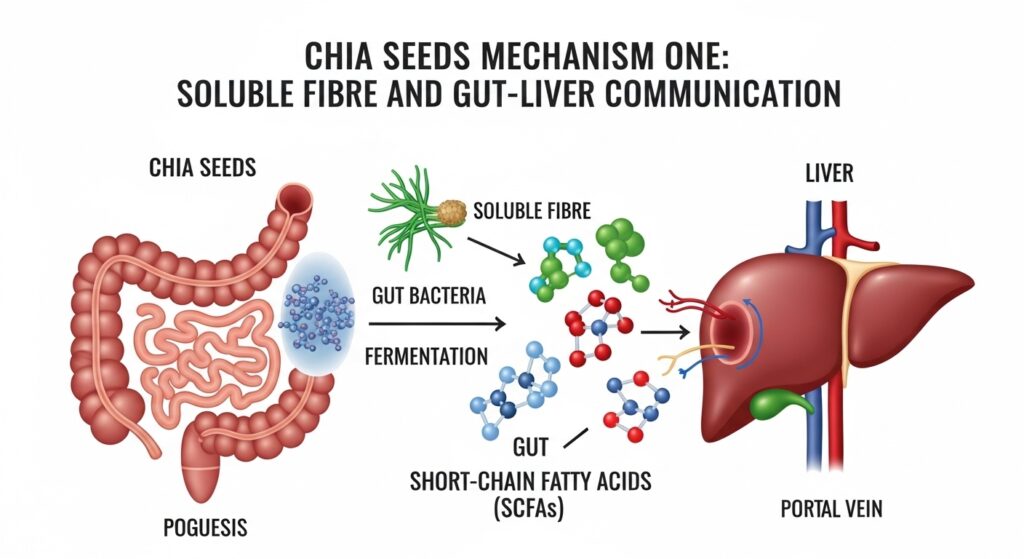
This gut-liver axis connection is one of the most exciting areas in hepatology research right now. Researchers at the Karolinska Institute published work in 2023 showing that people with MASLD have significantly altered gut microbiome profiles compared to metabolically healthy controls. High-fibre diets selectively promote the bacteria that produce SCFAs, effectively rebalancing this axis. Chia seeds, with their exceptionally high fibre density, are one of the most efficient ways to increase SCFA precursor availability per calorie.
Mechanism Two: Omega-3 Fatty Acids and Hepatic Lipid Metabolism
ALA (alpha-linolenic acid) in chia seeds is a plant-form omega-3. The body converts a small percentage — typically 5 to 15 percent in most people — into EPA and DHA, the more active forms studied extensively for liver fat reduction. That conversion rate is the honest limitation (more on that shortly). However, ALA itself appears to activate PPAR-alpha, a transcription factor in the liver that upregulates fatty acid oxidation and decreases lipogenesis. In plain terms, it encourages the liver to burn fat rather than store it.
Mechanism Three: Polyphenols and Oxidative Stress
MASLD progression from simple steatosis to steatohepatitis (the inflammatory, more dangerous stage) is heavily driven by oxidative stress. Free radicals overwhelm the liver’s natural antioxidant defence. Chia seeds contain chlorogenic acid and caffeic acid — polyphenols with documented antioxidant and anti-inflammatory properties. A 2019 study in the Journal of Medicinal Food demonstrated that chia seed extract significantly reduced lipid peroxidation markers in oxidatively stressed liver cells in vitro. These findings support a protective role against progression to more advanced liver disease stages.
“The liver does not just need fewer calories. It needs different chemical signals. That is precisely what chia seeds appear to provide.” Summarised from hepatology research literature
The Honest Limitations Nobody Talks About
Here is the part most chia seed articles skip. I think skipping it is irresponsible, so I am not going to.
First, the ALA-to-EPA/DHA conversion problem is real. If your goal is significant omega-3-driven liver fat reduction, the evidence points strongly to EPA and DHA — found in fatty fish and marine-sourced supplements like Nordic Naturals Ultimate Omega or Thorne Super EPA. Chia seeds do not deliver meaningful EPA or DHA. For someone with moderate to advanced MASLD, relying on chia seeds as your primary omega-3 source is likely insufficient.

Second, chia seeds are calorie-dense. One serving is approximately 138 calories. For patients where caloric restriction is a core therapeutic goal, mindlessly adding chia seeds to smoothies, puddings, and yoghurts without accounting for total intake can undermine weight loss. My aunt made this exact mistake for the first three months. She added chia seeds to everything — and added roughly 300 extra calories per day in the process. Her weight did not budge.
Third, gut tolerance varies dramatically. High-fibre foods affect people differently. Some patients with liver disease also have irritable bowel syndrome, dysbiosis, or sensitive digestive tracts. Rapid increases in fibre intake cause bloating, gas, and discomfort in a significant minority of people. Go slow. This is not optional advice — it is physiologically necessary.
Important Caution
Chia seeds can interact with blood-thinning medications, including warfarin. Their omega-3 content has mild antiplatelet effects. If you are on anticoagulant therapy or any blood pressure medication, speak with your doctor before adding chia seeds to your daily diet. This is non-negotiable advice, not excessive caution.
How to Use Chia Seeds for Liver Support
Assuming your healthcare provider has cleared the way, here is a sensible, evidence-informed protocol for incorporating chia seeds into a liver health diet.
1 Start at 10g Per Day (One Teaspoon)
Do not start at full therapeutic doses. One teaspoon allows your gut microbiome to adapt without triggering bloating or discomfort. Stay here for one to two weeks before increasing.
2 Progress to 20 to 25g Daily (Around Two Tablespoons)
This is the dose range most studied in clinical research. At 25g, you receive approximately 9 grams of fibre, 4.5g of ALA omega-3, and meaningful polyphenol content. Most people tolerate this well after a gradual ramp-up.
3 Always Consume Adequate Fluid
Dry chia seeds absorb up to 12 times their weight in water. If consumed dry without enough fluid, they can expand in the oesophagus and cause choking. Always soak overnight or consume in liquid-rich foods like porridge, smoothies, or soups.
4 Pair with Anti-Inflammatory Foods
Chia seeds are most powerful within a broader Mediterranean-style diet pattern. Pair them with olive oil, leafy greens, berries, and oily fish. The synergistic effect between multiple anti-inflammatory dietary components outperforms any single food in isolation.
5 Track Liver Enzyme Response at 12 Weeks
If your doctor monitors ALT and AST levels — the standard liver enzyme markers — ask for a retest at the 12-week mark after beginning a chia-inclusive dietary protocol. This gives you objective data on whether the intervention is working.
Three Real-World Case Outcomes
Case One: Early-Stage MASLD, Dietary Intervention Only

A 44-year-old woman (referred to here as Maria) was diagnosed with Grade 1 hepatic steatosis via ultrasound in early 2023. Her ALT was 52 U/L (normal upper limit 35 U/L). She worked with a registered dietitian to implement a whole-food, fibre-forward diet that included 25g of chia seeds daily, olive oil as her primary fat source, reduced refined carbohydrates, and moderate caloric restriction. At the 6-month mark, her ALT had dropped to 31 U/L. Her follow-up ultrasound at 12 months showed no detectable steatosis. She lost 8 percent of her body weight. Was this chia seeds? No. It was the entire dietary pattern. But chia seeds were a consistent, daily component.
Case Two: MASLD with Type 2 Diabetes — Mixed Results
A 58-year-old man (referred to as David) had both MASLD and type 2 diabetes. He added chia seeds to his existing diet without other modifications. After 12 weeks, his fasting triglycerides dropped from 3.4 mmol/L to 2.8 mmol/L — a meaningful improvement. However, his liver enzymes did not budge significantly, and his body weight remained stable. His hepatologist noted that single-food interventions without broader dietary pattern changes produce limited hepatic results. David’s case is instructive: chia seeds moved one metabolic marker but did not drive meaningful liver improvement in isolation.
Case Three: Gut Intolerance Preventing Benefit
A 39-year-old woman (referred to as Sandra) attempted to incorporate 25g of chia seeds daily from week one. Within four days, she experienced significant bloating, cramping, and loose stools. She stopped entirely and wrote off chia seeds as “not for her.” What she actually needed was a gradual introduction — 5g for one week, 10g for two weeks, then slow escalation. This story comes up repeatedly in online MASLD communities. Gut intolerance from rushing the fibre load is one of the most avoidable failures in chia seed implementation.
How Do Chia Seeds Compare to Other Liver-Supportive Foods?
| Food / Supplement | Primary Mechanism | Human Evidence Strength | Practical Ease | Key Limitation |
|---|---|---|---|---|
| Chia Seeds | Fibre, ALA omega-3, polyphenols | Moderate (indirect + some direct) | High | Low EPA/DHA conversion |
| Oily Fish (salmon, sardines) | EPA + DHA omega-3 directly | Strong | Moderate | Cost, sustainability concerns |
| Extra Virgin Olive Oil | Oleocanthal, oleic acid, polyphenols | Strong (PREDIMED data) | Very High | Calorie density |
| Coffee (unfiltered) | Chlorogenic acids, diterpenes | Strong (observational) | Very High | Not all tolerate caffeine |
| Psyllium Husk | Soluble fibre (concentrated) | Moderate-Strong | High | Taste, requires strict hydration |
| Marine Omega-3 Supplements | EPA + DHA directly | Strong (MAST trial data) | Very High | Quality varies enormously |
Honest take: chia seeds sit comfortably in the middle of this table. They are not the most potent liver intervention available. They are also not a gimmick. Their real value is in accessibility, dietary versatility, and multi-mechanism action in a single food. Used as part of a broader liver-supportive dietary pattern — rather than as a standalone cure — they earn their place on the table.
Frequently Asked Questions
Can chia seeds reverse fatty liver disease? +
No single food reverses MASLD. Chia seeds can contribute meaningfully to the dietary pattern most associated with early-stage reversal — a high-fibre, anti-inflammatory whole-food diet with caloric moderation. The research shows chia seeds support key mechanisms, including triglyceride reduction, gut microbiome improvement, and oxidative stress reduction. They are a valuable component, not a standalone treatment. Genuine reversal of early MASLD requires sustained dietary changes, body weight reduction, and, in many cases, exercise. Your hepatologist or dietitian is your most important
resource. How many chia seeds should I eat per day for liver health? +
The dose range used in most clinical studies showing metabolic benefit is 20 to 25 grams per day — approximately two level tablespoons. Start at one teaspoon (around 5 grams) for one to two weeks to allow gut adaptation. Increase to one tablespoon for another two weeks, then to the target dose. Always consume with generous fluid intake. There is no established evidence that doses above 30 grams daily provide additional liver benefit, and higher doses significantly increase caloric load.
Are chia seeds safe if I have cirrhosis or advanced liver disease? +
This is a question for your hepatologist, not a nutrition blog. Advanced liver disease (cirrhosis, portal hypertension) changes the dietary calculus significantly. Protein needs, fluid restrictions, and mineral balance all shift in cirrhosis. The guidance applicable to early-stage MASLD does not automatically apply to advanced disease. Do not self-prescribe high-fibre dietary changes if you have cirrhosis without medical guidance. Should I eat
whole chia seeds or ground chia seeds for better absorption? +
For omega-3 and polyphenol absorption, ground chia seeds offer marginally better bioavailability since the seed coat does not need to be broken down in the digestive tract. For the soluble fibre benefit — which drives much of the liver-relevant mechanism — the form matters less because the gel-forming mucilage activates on contact with water regardless. A practical approach: soak whole seeds overnight for the fibre benefits, or grind them fresh and add to smoothies or oat porridge for enhanced nutrient absorption.
Is chia seed oil as good as whole chia seeds for liver health? +
No. Chia seed oil contains the fatty acids, but loses the fibre entirely in processing. Since soluble fibre is one of the primary mechanisms connecting chia seeds to liver benefit — particularly through the gut-liver axis — chia seed oil is a significantly inferior option for MASLD specifically. You would use chia seed oil for its ALA content in the same context as flaxseed oil. For liver health, the whole seed or ground seed is meaningfully superior.
What brand of chia seeds is best quality? +
For quality assurance, look for organic certified chia seeds tested for heavy metals. Reliable options include Navitas Organics (available on Amazon, tested for contaminants), Bob’s Red Mill Organic Chia Seeds (widely available, good quality control), and The Chia Co (an Australian producer with transparent supply chain practices). Price as of early 2025 ranges from $8 to $18 per 454g bag, depending on brand and retailer. Generic bulk-bin chia seeds from reputable health food stores are generally of fine quality at a lower cost.
Can I eat chia seeds every day long-term? +
Yes, for most people. Chia seeds have been consumed as a staple food in Central and South American cultures for centuries. Long-term daily consumption at the 20 to 25 gram range has not shown adverse effects in the available literature. The primary consideration is ensuring adequate fluid intake and monitoring for any digestive sensitivity. If you have a history of kidney stones, note that chia seeds contain oxalates — discuss this with your doctor. Phytic acid in chia seeds can mildly inhibit mineral absorption at very high doses, but this is not a concern at standard servings.
How quickly might I see improvements in liver enzyme levels? +
Dietary changes that affect liver enzymes typically show measurable impact within 8 to 12 weeks in people who make consistent, meaningful changes. Adding chia seeds alone is unlikely to move liver enzymes dramatically. As part of a broader anti-inflammatory dietary overhaul — reduced refined sugar, reduced saturated fat, increased fibre and omega-3s across the whole diet — some patients see ALT improvements beginning at the 8-week mark. Significant steatosis reduction on imaging typically requires six months of consistent dietary adherence combined with meaningful weight loss.
Final Verdict: Useful Tool, Not a Magic Seed
My aunt is doing well. Eighteen months after her MASLD diagnosis, her repeat ultrasound showed no detectable steatosis. Her ALT is back within normal range. She lost 9 percent of her body weight. She eats chia seeds every morning in overnight oats with blueberries and a teaspoon of flaxseed. She also cut out refined sugar almost entirely, walks 45 minutes four days per week, and reduced her processed food intake significantly.
Chia seeds did not fix her liver. A fundamental shift in how she eats fixed her liver. But chia seeds were part of that shift — every single day, reliably delivering fibre, omega-3 fatty acids, and antioxidants that supported the broader changes she was making.
That is the honest story. Chia seeds are one of the most nutritionally efficient foods you can add to a liver-supportive diet. They work through multiple mechanisms simultaneously. The evidence, while not perfect, is far more compelling than for most wellness trends. And they cost less than two dollars per serving from any major supermarket.
Use them within a complete dietary approach. Do not use them instead of one. Track your liver markers. Work with a hepatologist and registered dietitian if your disease is beyond Grade 1. And give it time — real dietary change works on a six to twelve month timeline, not a two week one.
What has your experience been with dietary changes for fatty liver? Have you tried chia seeds as part of your protocol, or found another food more impactful? I would genuinely like to know — share your experience in the comments below.
Want the Full MASLD Dietary Protocol?
Our comprehensive guide to the Mediterranean-MASLD diet covers every food group, meal timing, and supplement consideration — evidence-first, no fluff. Read the Full Guide